Join me in challenging stigma, building awareness, and creating community for over 110,000 Canadians living with Parkinson’s.
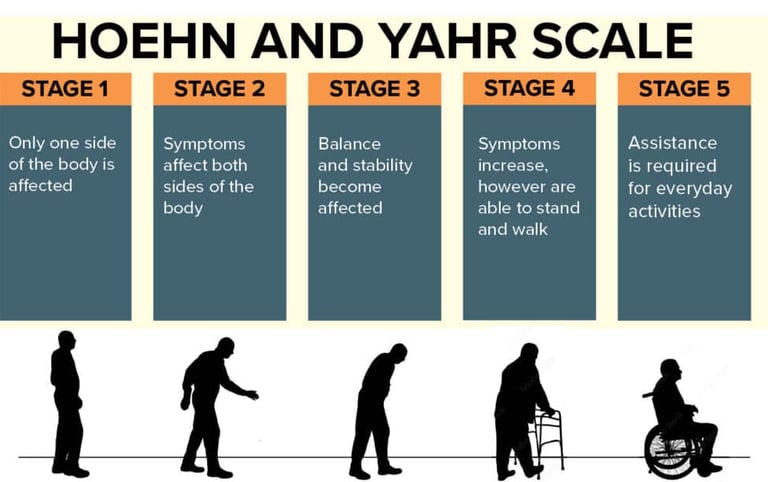
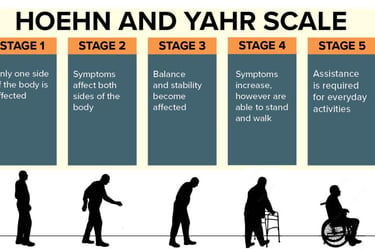
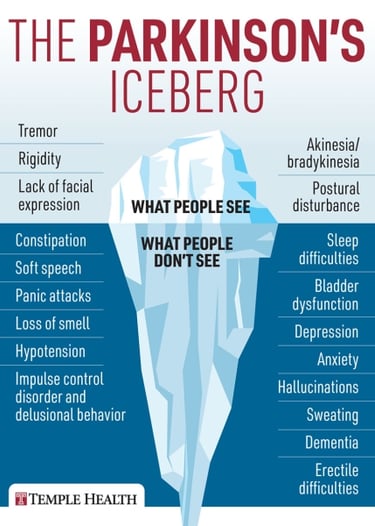
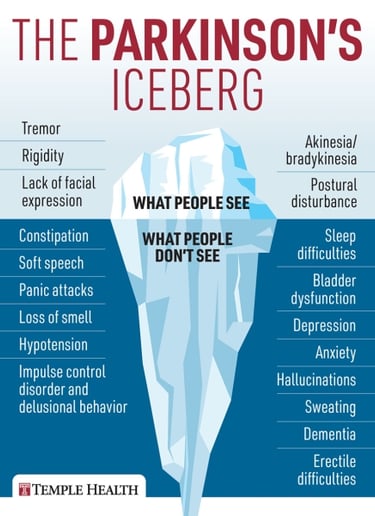
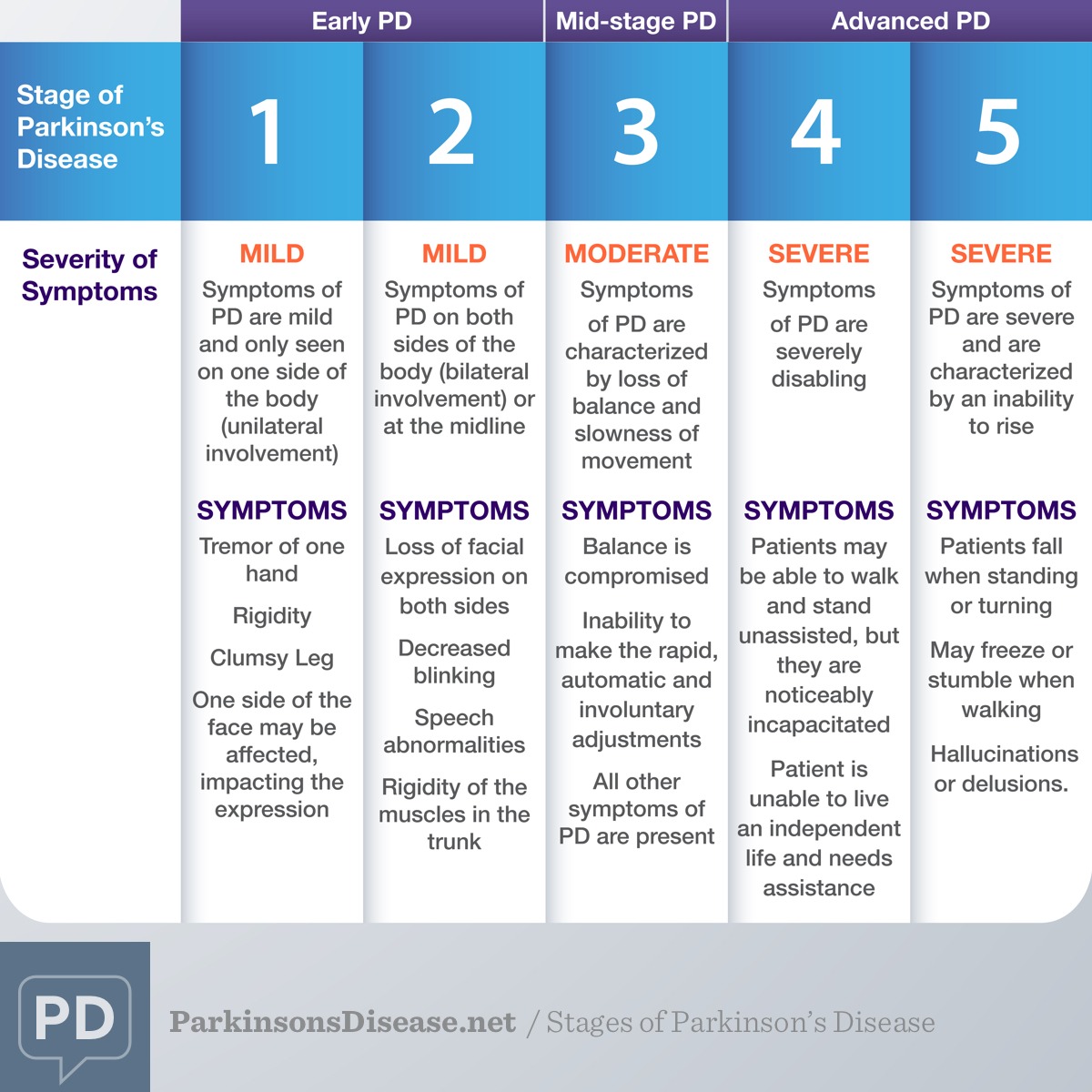
Parkinson's symptoms can range from tremors and stiffness to balance issues and slowed movement. Some people might experience cognitive changes or mood disorders. The progression can also vary greatly, with some people experiencing a slow onset and others noticing more rapid changes. It's truly unique for everyone.
You will often hear
"If you've met one person with Parkinson's, you've met one person with Parkinson's "
10 Early Signs
Know how to recognize the most common early symptoms of Parkinson's.



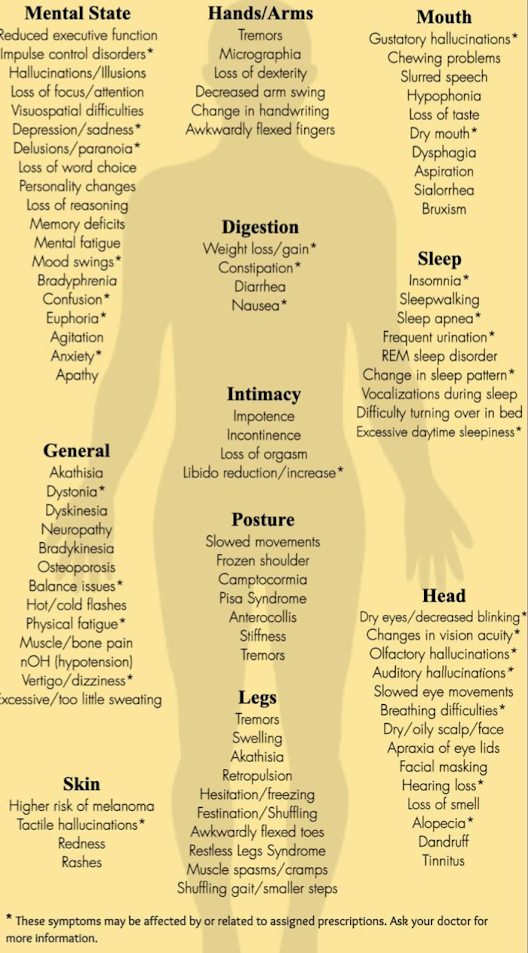
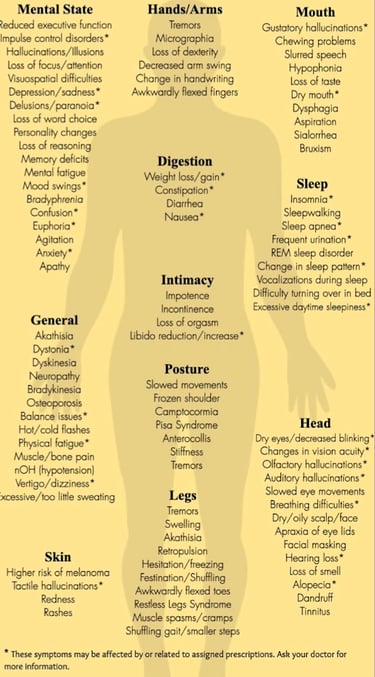
Parkinson's disease has both motor and non-motor symptoms:
Motor symptoms
These include:
Bradykinesia, or slow movement
Resting tremor
Rigidity
Walking or gait difficulty
Dystonia
Speech problems
Swallowing issues
Non-motor symptoms
These include:
Depression and other mood problems
Cognitive issues
Constipation and other gastrointestinal problems
Fatigue
Freezing
Hallucinations and delusions
Incontinence
Low blood pressure problems
Sleep problems
Other issues such as pain, sexual dysfunction, and vision changes
Non-motor symptoms can appear years or decades before motor symptoms, and can be vague. Early detection of non-motor symptoms can help with diagnosis and improve prognosis.
Parkinson’s disease (PD) can impact you emotionally. While PD is known to influence many aspects of movement, Parkinson's Outcomes Project research shows that two non-motor symptoms — anxiety and depression — play a key role in the disease and have the greatest impact on overall health. Fortunately there are proven strategies, including mindfulness meditation and exercise, that can help manage anxiety.
Depression
Caring for mental health is extremely important in Parkinson's disease (PD). Research estimates that at least 50% of people with PD will experience some form of depression during their Parkinson's journey and up to 40% will experience an anxiety disorder.
While everyone feels sad from time to time — and while people with PD may experience grief in reaction to a PD diagnosis — depression is different. Unlike sadness, which is temporary, depression can last for weeks or longer. Depression is a part of Parkinson's itself, resulting from PD-related changes in brain chemistry. Parkinson's impacts areas of the brain that produce dopamine, norepinephrine and serotonin — chemicals involved in regulating mood, energy, motivation, appetite and sleep.
Depression, while common in PD, is often overlooked and undertreated. Treating it is one of the most significant ways to decrease disability and improve quality of life.
A person may experience depression at any time in the course of PD, even before diagnosis. In addition, depression symptoms may come and go. It’s important to know that depression can intensify both movement and cognitive Parkinson's symptoms. Just as medications can improve tremors and other Parkinson's movement symptoms, they can also alleviate depression.
Discuss treatment options with your doctor. Researchers have found that people with Parkinson's who experience depression begin medications for motor symptoms earlier.
How is depression diagnosed?
Diagnosis is vital to effective treatment and recovery. A person must experience one of the following symptoms most of the time over the previous two weeks:
Depressed mood
Loss of interest or pleasure in activities once enjoyed
In addition, some of the following symptoms must be present:
Changes in sleep or appetite
Decreased concentration or attention problems
Increased fatigue
Feeling slowed down or restless
Feeling worthless and guilty
Suicidal thoughts or a wish for death
Anxiety
Feeling worried is an understandable reaction to a Parkinson’s diagnosis. But when feelings of constant worry or nervousness go beyond what is understandable, a person may be experiencing anxiety, which is more serious.
Types of Anxiety
Anxiety is not simply a reaction to a Parkinson’s diagnosis, but is instead a part of the disease itself, caused by changes in the brain chemistry of the brain. As many as two out of five people with PD will experience one of these forms of anxiety:
Generalized Anxiety Disorder
Anxiety Attacks
Social Avoidance
Obsessive-Compulsive Disorder (OCD)
Anxiety is not tied to disease progression — it can begin before a PD diagnosis or develop much later. Additionally, while some people with Parkinson's experience anxiety on its own, many are diagnosed with anxiety along with depression. If left unchecked, anxiety can worsen a person’s overall health condition.
How is anxiety diagnosed?
Anxiety is usually diagnosed by a primary care physician or a mental health professional who will ask questions about certain symptoms, mood changes and behaviors. A person living with anxiety can experience symptoms so intense that it makes daily living difficult.
Symptoms of anxiety can include:
Excessive fear and worry
Uncontrollable or unwanted thoughts
Sudden waves of terror
Nightmares
Ritualistic behaviors
Problems sleeping
Pounding heart
Cold and sweaty hands
Dizziness
Nausea
An anxiety disorder diagnosis is made in Parkinson's only if signs are not easily confused with movement symptoms and there is clear change from a person's previous behavior. For example, even though someone may have a legitimate concern that a tremor or change in walking ability may be noticed in public, a social avoidance diagnosis is only made if the concern is excessive, social situations are avoided and the anxiety interferes with social or work life.
Apathy
Apathy describes a lack of interest, enthusiasm or motivation. It interferes with the effective management of Parkinson’s disease (PD) symptoms, since apathetic people are less inclined to do things like exercise and follow their medication schedules.
You may be experiencing apathy if you feel that it is increasingly harder to get up and participate in life’s activities. Report this to your health care provider and work with your team to determine the best course of action.
In addition to apathy, people with PD also commonly experience depression and fatigue. Apathy is not the same as depression. In some cases, apathy is part of a depressive disorder or related to cognitive decline. Apathy coupled with depression can diminish a person’s energy and make it difficult to separate how each affects a person’s mood. Depression brings about feelings of worthlessness or guilt, whereas a person with apathy feels no mood or emotionally flat.
Apathy can be frustrating for people with PD, care partners and loved ones. Understanding apathy as a symptom of PD and finding ways to cope with it are key to ensuring a good quality of life and for maintaining good relationships with caregivers, family and friends.
Apathy and Care Partners
Apathy can be one of the most frustrating Parkinson’s symptoms a loved one or care partner will encounter. Research has shown that people with apathy require more from their care partners. It is difficult to see your loved one ignore or refuse to do things you both know are helpful for his or her Parkinson’s, such as exercise. Remember that apathy is a symptom of the disease and the person with PD is not necessarily being lazy or making excuses.